|
This is an essential contribution to the individual action plans and eventual patient outcomes. This method makes use of their skills and knowledge to provide data. The model demonstrates professional respect for the clinical expertise, knowledge and skills brought to the ward by the nurse consultant and provides opportunities for informal teaching and work-based learning. An entire ward of 20 patients can be discussed on a regular basis. Our model of continence service provides the opportunity for clinical consultancy on a large scale. Rehabilitation is the key to success for this client group who not only have bladder and bowel dysfunction but often other disabilities which they and their families find very distressing. Many have incurable conditions and diseases that impact on their activities of daily living and hence their quality of life. The majority of patients have some degree of bladder and or bowel dysfunction. Some of these are used more often in combination. Reviewing and prescribing medication is one of the most common aspects of our interventions - We have identified the range of interventions used on patients with bladder and bowel dysfunction. Sometimes nursing students are present - Using a specifically designed monitoring form completed by night staff, we review the previous seven nights' activity on average for about 16 patients - During the meeting we agree interventions for each individual and document and produce an action plan. This model of continence service has emerged to meet patient need: - Regular ward meetings are held most Fridays for about one hour - These meetings include the nurse consultant in bladder and bowel dysfunction, the ward manager/sister and the registrar. 
The long-term implications of incontinence after a stroke will affect the outcomes. Gebler et al (1993) classified incontinence after stroke into three: urge incontinence related to an overactive bladder (detrusor hyper reflexia), functional incontinence caused by cognitive or communication problems and overflow incontinence caused by hyporeflexia or medication. Burney et al (1996) identified that urinary retention was also common following an acute stroke, although this resolved with time. Ten years later confirmation is still being found that incontinence is common and that urinary incontinence has a negative impact on outcome (Ween et al, 1996). Borrie et al (1986) described that at one week post-stroke 60% were incontinent - a poor prognostic indicator that was also linked strongly with mental impairment, motor deficit and impaired mobility. Incontinence was more common in those patients who were also dependent and immobile. Brocklehurst et al (1985) found that out of 135 stroke patients 40% were incontinent within the first two weeks of diagnosis and 24% were still incontinent a year later. Incontinence is common following a stroke and recognised as a poor prognostic indicator (Wade and Langton-Hewer, 1985 Jongbloed, 1986). Three years on, a sustainable model of continence service has emerged which has become accepted, established and valued. Before the opening of the ward the continence service was invited to consider their involvement in this new venture. Our 20-bed ward serves three consultants (neurology, rehabilitation and stroke), with 15 beds for stroke patients and five for neurology/rehabilitation. 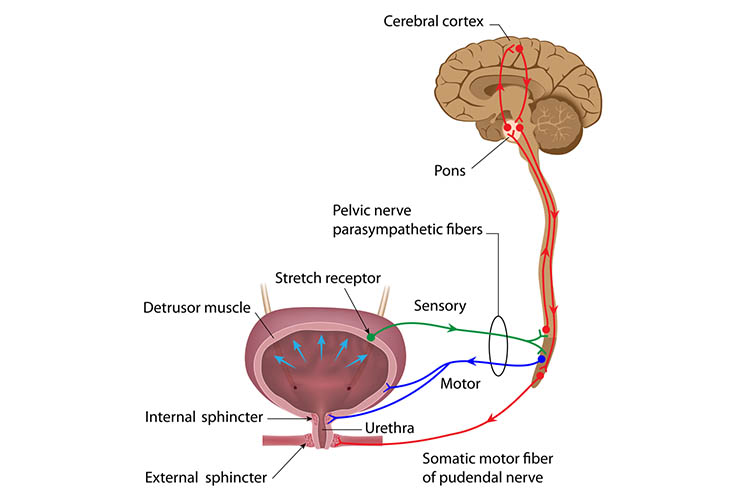
Lizzie Dodd, RN, is ward manager Frank McGurrin, RMN, RN, DMS, MBIB, MBA, is director of nursing/deputy chief executive Jumoke Abili is a registrar, andValerie Jones is stroke consultant, Mayday University Hospital, Croydon, Surrey Ray Addison, RN, FETC, Cert.H.Ed, BSc, is is nurse consultant, bladder and bowel dysfunction at Mayday University Hospital, Croydon, Surrey
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
